Light-Weight Localization and Scale-Independent Multi-gate UNET Segmentation of Left and Right Ventricles in MRI Images
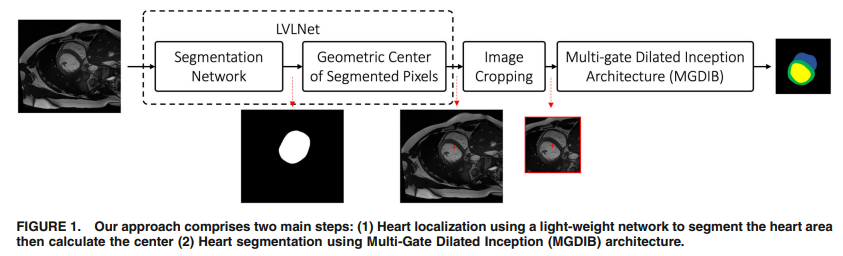
Purpose: Heart segmentation in cardiac magnetic resonance images is heavily used during the assessment of left ventricle global function. Automation of the segmentation is crucial to standardize the analysis. This study aims at developing a CNN-based framework to aid the clinical measurements of the left ventricle and right ventricle in cardiac magnetic resonance images. Methods: We propose a fully automated framework for localization and segmentation of the left ventricle and right ventricle in both short- and long-axis views from cardiac magnetic resonance images. The localization module utilizes a light-weight model that detects the region of interest and feeds it to the segmentation model. Also, we propose the Multi-Gate block as an extension to the UNet to boost the segmentation performance by aggregating multi-scale features. Comparison between our proposed method and the baseline UNet was performed to show the gain in the overall performance. The reliability of the model was assessed by testing the method against cardiac magnetic resonance images with different levels of noise and deformations. Results: Heart localization accuracy was 0.59 and 1.75 pixels in both short- and long-axis views respectively. Left and right ventricle blood-pool segmentation Dice was (0.93, 0.90) in end-systole and (0.97, 0.95) in end-diastole. The left ventricle myocardium was segmented accurately with Dice of 0.91 and 0.90 in end-systole and end-diastole respectively. Left ventricle ejection fraction was found to be highly correlated with the gold standard with r = 0.987. Moreover, the proposed pipeline is fast, achieving 0.002 sec per image on average. Conclusion: Adding the Multi-Gate Dilated Inception Block has boosted the performance of UNet architecture and has shown generalization ability when tested on noisy and deformed cardiac magnetic resonance images. The proposed method has proven its wide applicability and reliability for heart detection when tested on different datasets. © 2021, Biomedical Engineering Society.